THE SCIENCE BEHIND REDUCOSE®
Opting for a balanced, adequate and varied diet is important for maintaining a happy and healthy lifestyle. A healthy diet can help protect the human body against certain diseases, especially non-communicable diseases such as obesity, diabetes, heart disease and some cancers. Consuming whole foods and a low glycemic index diet is an important facet of healthy eating and a healthy lifestyle The high-paced modern lifestyle can make it difficult to maintain a balanced, healthy diet with many people consuming high glycemic index carbohydrates (the so called, fast carbs) in large quantities. Diets like this are considered unhealthy as the carbohydrates are not only energy dense foods, but also promote fat storage and hunger.
How it works
Blood Sugar Basics
Dietary carbohydrates are classified as either sugars, starches or fibers and are defined by their ease of digestibility and the length of their saccharide chain (the number of basic carbohydrate units such as glucose). These chains can vary in length from short chains of two units, such as sucrose or table sugar, to chains containing hundreds of thousands of saccharide units such as starch and fiber.
Starches are further classified based on their speed of digestion: rapidly digestible starch (RDS), slowly digestible starch (SDS), or resistant starch (RS). When we eat these different starches they have markedly different effects on our blood sugar levels. Rapidly-digestible starch is quickly broken-down and causes a rapid increase in our blood sugar levels after eating a meal. In contrast, resistant starches and fiber escape digestion in the small intestine and pass into the large intestine where it becomes food for the microbiome.

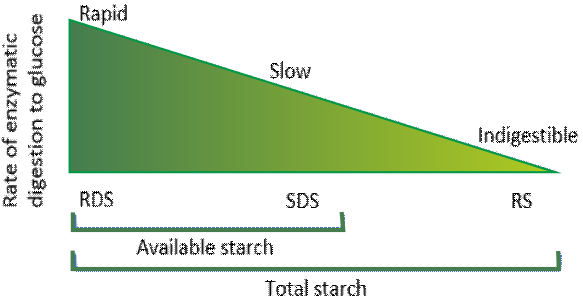
Related to the rate of carbohydrate digestion is the glycemic index (GI), a relative ranking system for carbohydrate foods and their impact on our blood sugar levels. Carbohydrates with a high GI value have a dramatic influence on our postprandial blood sugar levels and eating them releases a large amount of glucose rapidly into the bloodstream. Many people are unaware that sugar is a medium GI carbohydrate, and gram for gram, refined starches have twice the glycemic impact of sugar. Conversely, a low GI diet leads to low and slow changes in postprandial blood sugar levels and have been clinically demonstrated to improve blood sugar profile, blood lipids profile, and insulin resistance.
Surprisingly gram for gram, refined starches have 2X the glycemic impact of sugar
Benefits beyond healthier blood glucose
The effect of Reducose® in lowering postprandial blood glucose by preventing the digestion of carbohydrates, triggers a cascade of positive health effects, many of which support maintaining a healthy body weight and BMI.* The undigested carbohydrates will remain in the gut lumen and continue travelling down the small intestine. Once they reach the ileum, the last part of the small intestine, they trigger what’s termed the ileal brake
The ileal brake is a nutrient-triggered inhibitory feedback mechanism that induces satiety. When macronutrients bind to receptors in the ileum, the ileal brake is triggered resulting in a slowing of upper gut motility, reduced appetite, and delayed gastric emptying.
Linked to the ileal brake is the second meal effect. The second meal effect is a phenomenon where the GI of one meal can influence the glycemic response to a subsequent meal. Having a low GI intake in one meal lowers the postprandial glycemic response in a subsequent meal. This effect is thought to be mediated through several interacting mechanisms, including through the actions of incretin hormones (GLP-1 & GIP) and by the fermentation of undigested carbohydrates to short-chain fatty acids by the microbiome and their subsequent absorption.
The benefits of the second meal effect, whilst observable as a lower postprandial glucose response, extends to weight management. The second meal effect increases the rate of fat oxidation and favors the use of fat to meet the body’s energy requirements, whilst people who eat high GI meals favor fat storage and the use of carbohydrates for energy.
One of the benefits of the second meal effect is how it potentially helps with weight loss. The glucose response after eating the initial low GI meal, and the resultant lower glucose response from the second meal effect results in the body’s insulin response being moderated down.
Insulin’s primary function is to stimulate cells to remove glucose from the blood to maintain glucose homeostasis. As glucose is an important energy source for the body, any excess glucose is stored initially as glycogen, and then as fat, and this process is also mediated by insulin.
High GI foods cause sharp spikes in blood glucose, with a resultant excess production of insulin. This excess insulin puts the body into fat storage mode and calories that would normally be used immediately for energy as carbohydrates are now stored as fat. In order to lose weight, it is therefore important to have a moderate insulin response. This is achieved through eating low GI meals, and data shows that low GI meals not only reduce the glycemic response, but also improve appetite control and enhance fat oxidation.
In addition to preventing glucose calories getting into the body, Reducose® has been shown to significantly lower insulin response after consuming carbohydrates and turns high GI foods into low GI ones, helping to put the body into fat burning mode.* Reducose® may stimulate the ileal brake, increasing satiety and trigger the second meal effect, further supporting healthy weight loss.*
Reducose® is clinically shown to lower blood glucose response & the glycemic index of foods
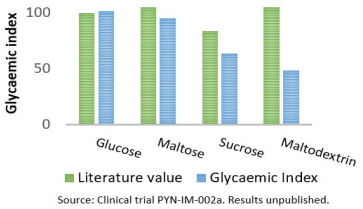
In a clinical trial conducted by Phynova, a single 250mg dose of Reducose® was incorporated directly into common dietary carbohydrates and given to healthy individuals. Reducose® caused a significant reduction in the glycemic index of the test carbohydrates. The greatest effect was seen with maltodextrin, a long chain carbohydrate made from corn starch, where Reducose® lowered the GI of the maltodextrin by 55%. These findings were replicated in a second clinical trial, the results of which have been published (Wang et al., 2018). This reduction in glycemic index of foods results in significant lowering in postprandial blood glucose levels.*
In two published clinical studies Reducose® was shown to lower postprandial blood glucose and postprandial plasma insulin following a carbohydrate challenge (sucrose in one study, maltodextrin in the second). These studies showed that Reducose® lowered the postprandial blood glucose levels by up to 42% (Lown et al., 2017; Thondre et al., 2021). Reducose® also lowered the postprandial insulin response by a corresponding amount (-41%). The clinical studies reported no adverse events and in a gastrointestinal symptoms questionnaire, there was no difference between Reducose® and placebo in incidence or severity of GI side-effects.
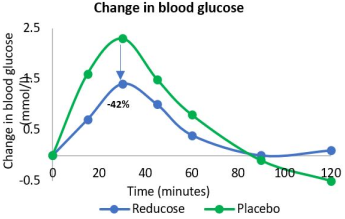
Reducose® demonstrates a classical dose response curve with significant effects over placebo. Importantly, we did not find any significant differences between the treatment groups in the odds of experiencing one or more gastrointestinal symptoms.
LOWN ET AL PLOS ONE. 2017

References








